Breast Cancer
 Breast cancer happens when normal cells in the breast change and grow out of control. These cancer cells not only cause a tumor in the breast tissue, they also have the capacity to spread to other organs such as lungs, liver and bone. Women sometimes discover they have breast cancer because they find a lump in one of their breasts.
Breast cancer happens when normal cells in the breast change and grow out of control. These cancer cells not only cause a tumor in the breast tissue, they also have the capacity to spread to other organs such as lungs, liver and bone. Women sometimes discover they have breast cancer because they find a lump in one of their breasts.
Risk factors for developing breast cancer
Risk factors refer to the chance that a person has to develop breast cancer. Having a risk factor or several risk factors does not mean a person will get the disease; the chances are only slightly higher than in the average person. It is important to know that every woman is at risk.
Known risk factors
- Gender: Women are 100 times more likely to get breast cancer than men
- Age: The risk of breast cancer increases with age
- Family history: A woman’s risk of breast cancer approximately doubles if she has a first-degree relative (mother, sister, daughter) who has been diagnosed with breast cancer. There is a higher risk for breast cancer if there is a history of a close relative who has had breast, uterine, ovarian, or colon cancer.
About 20-30% of women with breast cancer have a family history of the disease. Some people have abnormal genes that make them more likely to develop breast cancer. The most common gene defects are found in the BRCA1 and BRCA2 genes. These genes normally produce proteins that protect one from cancer.
Women with the gene defect (mutation) have up to an 80% chance of getting breast cancer during her life.
About 5-10% of breast cancers are thought to be caused by these inherited gene mutations (abnormal changes passed through families).
- Menstrual cycle: Women who started their menstrual cycle before age 12 and develop menopause late – after age 55 – have an increased risk.
- Alcohol use: Alcohol causes genetic damage and increases oestrogen and other hormones associated in development of breast cancer.
- Childbirth: Women who never had children or who had children after age 30 have an increased risk.
- Oestrogen exposure: Women who receive hormone replacement therapy (HRT) for several years are at increased risk.
- Radiation: Persons who had radiation therapy to their chest at young age are at increased risk, especially radiation therapy for Hodgkin’s lymphoma.
- Breast density: Dense breast tissue means there is more gland tissue and less fatty tissue, this increases the risk.
Signs and Symptoms
In the early stages of breast cancer there may be no signs or symptoms. As the cancer grows and enlarges you may experience any of these changes:
- A breast lump or thickening that feels different from the surrounding tissue
- Fluid other than breast milk discharging from the nipple e.g. blood
- Change in the size or shape of a breast
- Changes to the skin over the breast, such as dimpling
- Inverted nipple (pulled back into the breast)
- Peeling, scaling or flaking of the nipple or breast skin
- Redness or pitting of the skin over your breast, like the skin of an orange

Breast cancer screening methods
Breast-self-exam
Breast self-examination is a way of finding changes in your own breasts. You should become familiar with how your breasts look and feel, so that one can notice differences over time. The best time to do a breast self-examination is a week after your period ends. If you no longer get your periods, you can exam at any time. Consider examining yourself once a month.
Step by step
- Stand in front of a mirror and place both hands at your side. Look at the breast shape, nipples, skin colour and texture and check for dents.
- Lift your your hand over you head and turn to the side. Then look at each whole breast in the mirror. Lift your breast up to see the skin underneath.
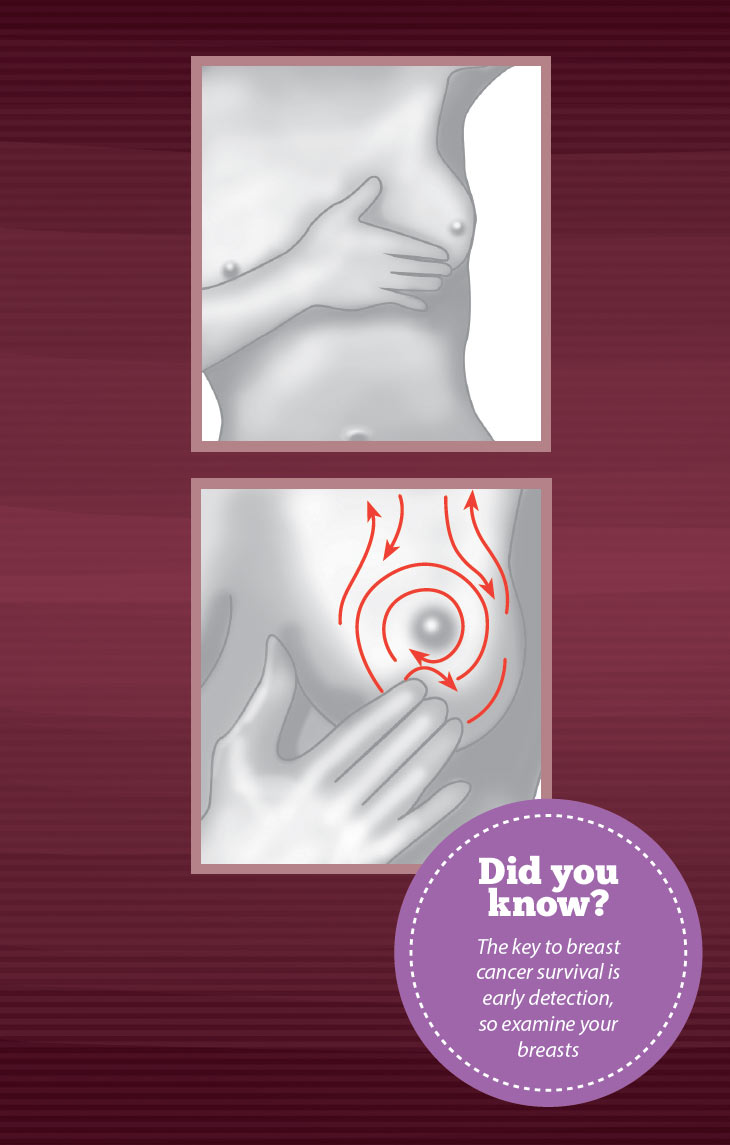
- Lie down and put you left hand above your head. This flattens the breast and makes it easier to examine. Use your right hand to examine your left breast. Start in the upper breast near the arm pit and go up and down across the breast.
- Do the examination by making small circles with the pads (not finger tips) of your three middle fingers. Move your fingers in circles. At each spot on the breast, make three circles: one very light, one a bit firmer into the breast, and one deep in the breast. Then feel above and below the collarbone and the underarm areas for swelling. Then switch hands and do the same thing on the other breast.
- It is normal to feel your ribs in your chest. Abnormal lumps feel firm, have irregular edges and sometimes feel like they are “stuck” to your chest. If you are not sure if the lump is significant, see your doctor for an examination.
Mammogram
A mammogram is a breast x-ray. The breast is pressed between two plates and x-rays are used to take pictures of breast tissue. It is the best screening test available to detect breast cancer before a lump is palpable.
When to start screening with mammogram
Screening is recommended from the age of 40 onwards. There is some controversy surrounding starting before age 50 as the chances for having breast cancer is less common and that may result in a large number of women that will be investigated unnecessarily. Mammograms are less likely to find breast tumors in women younger than in women older than 50 years.
Your decision to have or delay mammograms between ages 40 to 49 should be based on your individual preferences and risk of breast cancer. Screening with a mammogram is recommended once a year and after age 50 this test is recommended every second year.
Women who have screening mammograms have a lower chance of dying from breast cancer than women who do not have screening mammograms because the cancer is picked up early.
What if my mammogram is abnormal?
If your mammogram is abnormal, you will need further testing. In most cases, a woman with an abnormal mammogram does not have breast cancer. In 90% of women with an abnormal mammogram, breast cancer is not found.
The following investigations will evaluate the abnormality seen on a mammogram:
- Ultrasound exam of the breast tissue – this provides a clearer picture if a lump is suspected and can assist with taking a biopsy.
- Biopsy of the lump – this involves the removal of cells or tissues so that they can be viewed under a microscope by a pathologist to check for signs of cancer.
Treatment
Treatment of breast cancer depends on the type of breast cancer and the stage of the cancer i.e. the size of the tumor and whether it is in the breast only or has spread to lymph glands or other parts of the body. Treatments include surgery, chemotherapy, hormonal therapy, biological therapy and radiation.
Most patients get a combination of these therapies:
- Surgery – Breast cancer is usually treated with surgery to remove the cancer. Many women with breast cancer can choose between mastectomy and breast conserving therapy (also called “lumpectomy”). Mastectomy is surgery to remove the whole breast. Lumpectomy is surgery to remove the cancer and a section of healthy tissue around it. Women who choose this option keep their breast. But they usually must have radiation therapy after surgery.
- Radiation therapy – Radiation kills cancer cells. Radiation therapy uses high-powered beams of energy, such as X-rays, to kill cancer cells. External beam radiation is commonly used after lumpectomy for early-stage breast cancer. Doctors may also recommend radiation therapy after mastectomy for larger breast cancers or cancers that have spread to the lymph nodes.
- Chemotherapy – Chemotherapy is the term doctors use to describe a group of medicines that kill cancer cells. Some women take these medicines before surgery to shrink the cancer and make it easier to remove. Some women take these medicines after surgery to keep cancer from growing, spreading, or coming back.
- Hormone therapy – Some forms of breast cancer grow in response to hormones. Your doctor might give you treatments to block hormones or to prevent your body from making certain kinds of hormones. Doctors sometimes refer to these cancers as estrogen receptor positive (ER positive) and progesterone receptor positive (PR positive) cancers.
- Targeted therapy – Some medicines work only on cancers that have certain characteristics. Targeted drug treatments attack specific abnormalities within cancer cells. Your doctor might test you to see if you have a kind of cancer that would respond to this kind of therapy.
Life expectancy
Death rates from breast cancer has decreased significantly in the past 20 years due to treatment advances and earlier detection through screening and increased awareness.


